The festive season often brings to mind joyous gatherings, delicious feasts, and the comforting warmth of good company. However, for those navigating the challenges of diverticulitis, the thought of indulging in traditional holiday fare can sometimes spark anxiety. Understanding the right diverticulitis diet NHS UK recommendations is crucial for enjoying this time of year with comfort and confidence. This comprehensive guide, tailored to NHS UK guidelines, will empower you with the knowledge to make smart, nourishing choices, ensuring your celebrations are as enjoyable as they are healthy.
Understanding Diverticulitis: A Gentle Explanation
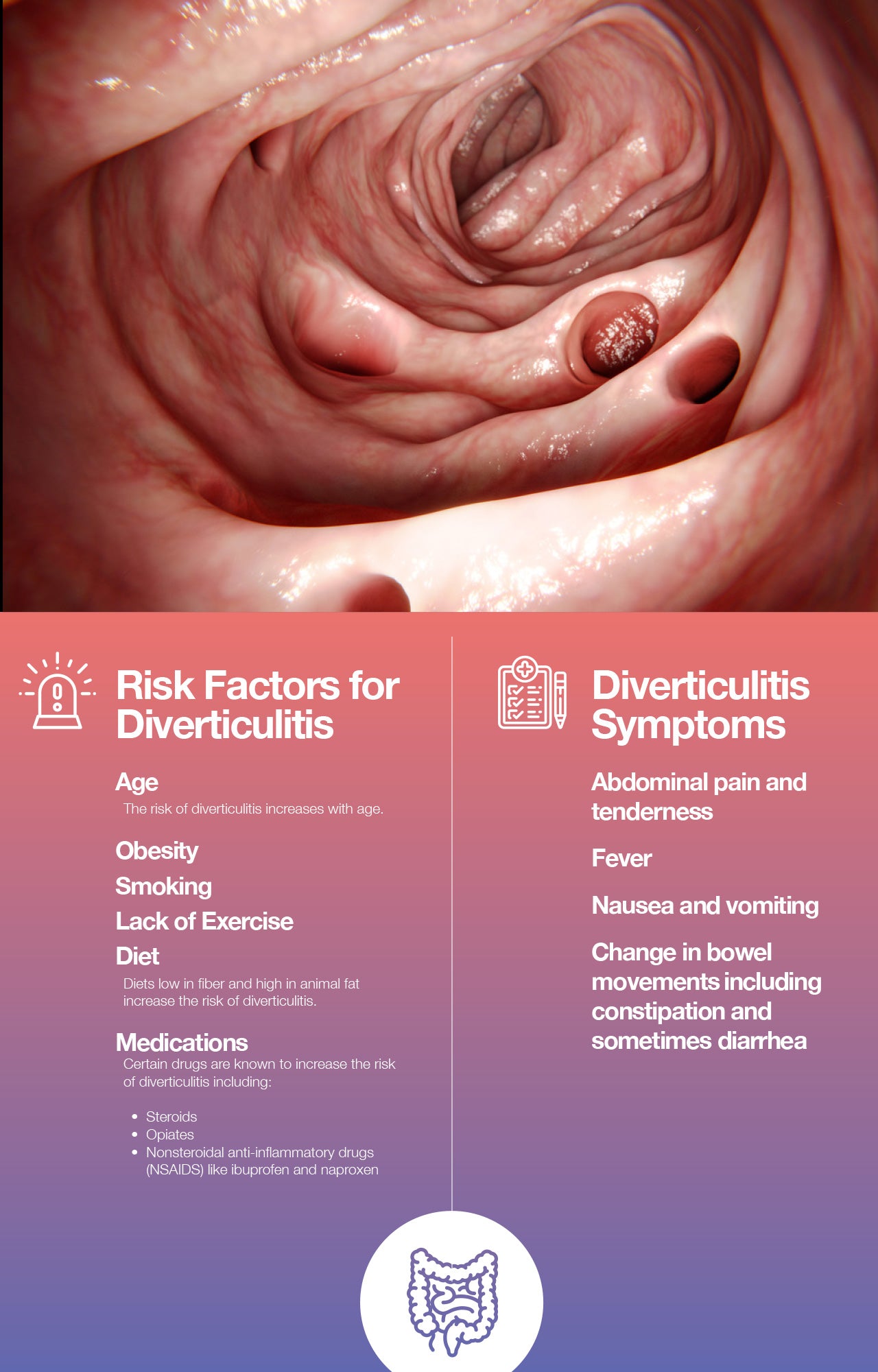
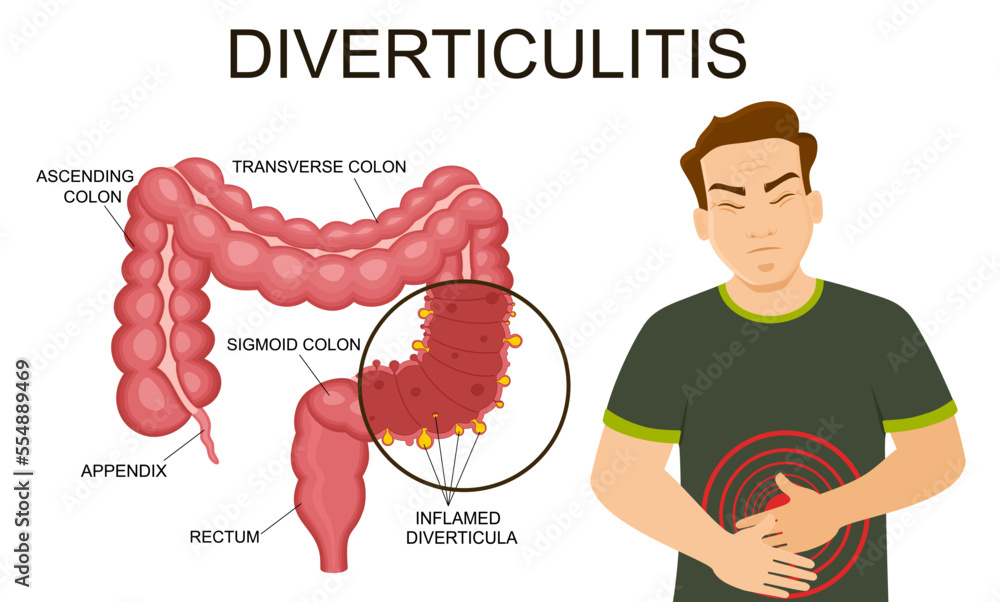
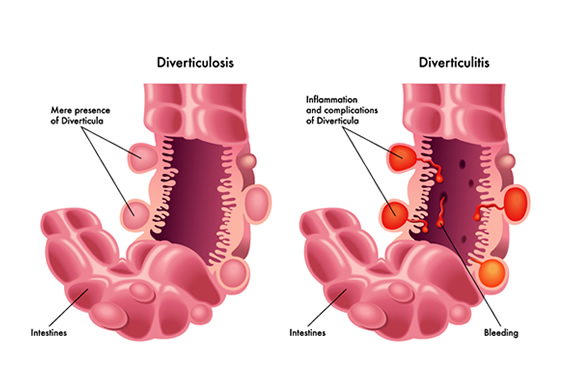
Before diving into dietary specifics, let’s briefly touch upon what diverticulitis is. Diverticula are small, bulging pouches that can form in the lining of your digestive system. When these pouches become inflamed or infected, it’s known as diverticulitis. While not everyone with diverticula develops diverticulitis, it’s a condition that can cause significant discomfort, including abdominal pain, bloating, and changes in bowel habits. The good news is that with the right approach to diet, many individuals can manage their symptoms effectively and even prevent future flare-ups.
The Cornerstone of Diverticulitis Management: Fibre
When it comes to a diverticulitis diet NHS UK guidance consistently emphasizes the vital role of dietary fibre. Fibre is a true hero for digestive health, and its impact on diverticulitis is profound.
Why Fibre is Your Festive Friend
Fibre acts like a gentle broom for your digestive tract. It adds bulk to your stools, making them softer and easier to pass. This, in turn, reduces the pressure within your colon, which is believed to be a key factor in preventing the formation and inflammation of diverticula.
- Soluble Fibre: This type of fibre dissolves in water to form a gel-like substance. It can help to soften stools and regulate blood sugar levels. Excellent sources include oats, barley, beans, lentils, apples, and citrus fruits.
- Insoluble Fibre: This type of fibre does not dissolve in water and adds bulk to the stool, promoting regular bowel movements. Whole grains, nuts, seeds, and the skins of many fruits and vegetables are rich in insoluble fibre.
Navigating Fibre Intake: A Gradual Approach
It’s essential to understand that while fibre is beneficial, a sudden increase can sometimes lead to gas and bloating, especially if your body isn’t accustomed to it. Therefore, the key is a gradual introduction and consistent intake.
- Start Slowly: If you’re new to a high-fibre diet, begin by adding one high-fibre food to your meals each day. For example, swap white bread for wholemeal bread, or add a handful of berries to your breakfast cereal.
- Hydration is Key: As you increase your fibre intake, it’s crucial to drink plenty of water. Water helps the fibre to move through your digestive system smoothly. Aim for at least 8 glasses of water a day, and more if you’re active or the weather is warm.
- Listen to Your Body: Pay attention to how your body responds. If you experience discomfort, ease back on the fibre intake and gradually reintroduce it.
Dietary Recommendations During a Diverticulitis Flare-Up
During an active diverticulitis flare-up, your digestive system needs a period of rest and recovery. The NHS UK typically advises a diverticulitis diet NHS UK that is low in fibre during this acute phase.
The Low-Fibre Phase: Gentle Nourishment
The goal here is to reduce the amount of undigested material passing through your colon, giving the inflamed areas a chance to heal.
- What to Eat:
- Refined Grains: White bread, white rice, plain pasta, and refined cereals (like cornflakes or puffed wheat).
- Cooked, Seedless Fruits: Peeled apples, pears, and bananas. Fruit juices without pulp are also generally well-tolerated.
- Cooked, Seedless Vegetables: Well-cooked and peeled vegetables like carrots, potatoes (without skin), and pumpkin. Strained vegetable juices can also be an option.
- Lean Proteins: Tender, well-cooked meats, poultry, and fish. Eggs are also a good choice.
- Dairy: Milk, yogurt, and cheese, provided you tolerate them well.
- What to Avoid:
- High-Fibre Foods: Whole grains, nuts, seeds, legumes (beans, lentils), raw fruits and vegetables with skins and seeds.
- Spicy Foods: These can sometimes irritate the digestive system.
- Fatty Foods: Fried foods, rich gravies, and fatty cuts of meat.
- Alcohol and Caffeine: These can be dehydrating and may irritate the gut.
Transitioning Back to a High-Fibre Diet
Once your symptoms have subsided, it’s vital to gradually reintroduce fibre to prevent future flare-ups. This transition should be slow and steady, guided by your body’s response.
- Start with Easily Digestible Fibres: Begin with cooked fruits and vegetables without skins or seeds, and gradually introduce whole grains.
- Monitor Your Symptoms: If you experience any discomfort, reduce your fibre intake slightly and try again later.
Long-Term Dietary Strategies for Diverticulitis Management
The most effective diverticulitis diet NHS UK strategy for long-term management focuses on a consistent, high-fibre intake, alongside other healthy eating principles.
Embracing a Fibre-Rich Lifestyle
Making fibre a regular part of your diet is the cornerstone of preventing diverticulitis recurrence.
- Whole Grains Galore: Make wholemeal bread, brown rice, oats, and quinoa staples in your kitchen.
- Fruit and Veggie Power: Aim for at least five portions of fruits and vegetables daily. Opt for a variety of colours and textures. Don’t shy away from the skins and seeds of fruits and vegetables unless advised otherwise by your doctor.
- Legume Love: Incorporate beans, lentils, and chickpeas into your meals. They are packed with fibre and protein.
- Nuts and Seeds: A small handful of nuts and seeds can provide a good dose of fibre and healthy fats.
Hydration: The Unsung Hero
We can’t stress this enough Low cholesterol diet meal plan printable your festive guide to a healthier heart – staying well-hydrated is paramount for a healthy digestive system, especially when managing diverticulitis. Water is your best friend. Herbal teas can also be a soothing and hydrating option.
Foods to Be Mindful Of (and Why)
While the old advice to avoid nuts, seeds, and popcorn has largely been debunked by modern research, some individuals may find that certain foods trigger their symptoms.
- Nuts, Seeds, and Popcorn: Historically, it was believed that these could get lodged in diverticula and cause inflammation. However, current evidence suggests this is rare. If you find they cause you discomfort, it’s perfectly acceptable to limit them.
- Red Meat: Some studies suggest a link between high red meat consumption and an increased risk of diverticulitis. Opting for leaner protein sources more often can be beneficial.
- Processed Foods: These are often low in fibre and high in unhealthy fats and sugar, which can contribute to inflammation and weight gain, both of which can exacerbate digestive issues.
The Importance of a Balanced Diet
Beyond fibre, a generally healthy and balanced diet supports overall well-being, including digestive health.
- Plenty of Fruits and Vegetables: Aim for a rainbow of colours to ensure a wide range of vitamins, minerals, and antioxidants.
- Lean Proteins: Fish, poultry, beans, and lentils are excellent choices.
- Healthy Fats: Avocados, olive oil, nuts, and seeds.
- Limit Sugary Drinks and Processed Foods: These offer little nutritional value and can contribute to inflammation.
Festive Feasting with Diverticulitis in Mind
The holiday season doesn’t have to mean dietary restrictions that dampen your spirits. With a little planning, you can enjoy delicious and festive meals while adhering to your diverticulitis diet NHS UK recommendations.
Smart Swaps for Festive Favourites
- Roast Dinner: Opt for lean cuts of turkey or chicken. Serve with plenty of roasted vegetables (carrots, parsnips, Brussels sprouts) and a generous portion of wholemeal stuffing. Choose gravy made with lean meat juices rather than fatty drippings.
- Christmas Pudding and Mince Pies: While these can be rich, enjoy them in moderation. Consider making or choosing versions that are less laden with suet or have added dried fruits for extra fibre.
- Cranberry Sauce: Homemade cranberry sauce is a fantastic way to incorporate fruit fibre.
- Vegetable Sides: Embrace a wide array of fibre-rich vegetables. Steamed or roasted broccoli, green beans, and kale are excellent choices.
- Desserts: Fruit-based desserts, such as baked apples with cinnamon or a berry compote, can be a lighter and more fibre-rich option.
Mindful Eating and Portion Control
Even with the best dietary choices, overindulging can still lead to digestive discomfort.
- Eat Slowly: Savour your food and allow your body time to signal fullness.
- Smaller, More Frequent Meals: If large meals feel overwhelming, consider having smaller portions more often.
- Listen to Your Body: If you know certain festive foods don’t agree with you, it’s okay to politely decline or opt for a smaller portion.
When to Seek Professional Advice
While this guide provides general information based on diverticulitis diet NHS UK principles, it’s crucial to remember that individual needs can vary.
- Consult Your Doctor or a Dietitian: If you are experiencing persistent symptoms, have concerns about your diet, or are unsure about the best approach for your specific situation, always consult with your GP or a registered dietitian. They can provide personalized advice and create a tailored dietary plan for you.
- Red Flags: Seek immediate medical attention if you experience severe abdominal pain, fever, chills, vomiting, or rectal bleeding, as these could indicate a more serious complication.
Conclusion: Embracing a Healthier, Happier You
Navigating a diverticulitis diet NHS UK doesn’t mean sacrificing the joy of good food, especially during festive times. By understanding the principles of fibre intake, making smart food choices, and listening to your body, you can enjoy delicious meals and maintain excellent digestive health. Embrace the knowledge, make gradual and sustainable changes, and celebrate the season with comfort and confidence.
Frequently Asked Questions (FAQ) about Diverticulitis Diet NHS UK
Q1: What is the most important dietary recommendation for diverticulitis according to the NHS UK?
A1: The most crucial recommendation from the NHS UK for diverticulitis management is a high-fibre diet to promote regular bowel movements and reduce pressure in the colon.
Q2: Should I avoid nuts, seeds, and popcorn if I have diverticulitis?
A2: Current NHS UK guidance suggests that most people with diverticulitis do not need to avoid nuts, seeds, or popcorn. However, if you find these foods trigger your symptoms, it’s advisable to limit them.
Q3: What should I eat during a diverticulitis flare-up?
A3: During a flare-up, the NHS UK typically recommends a low-fibre diet. This includes refined grains, cooked seedless fruits and vegetables, and lean proteins.
Q4: How much water should I drink with a high-fibre diet?
A4: It’s essential to drink plenty of water, aiming for at least 8 glasses a day, to help fibre move smoothly through your digestive system and prevent constipation.
Q5: Can I still enjoy festive foods if I have diverticulitis?
A5: Yes, you can! By making smart swaps, focusing on fibre-rich options like vegetables and whole grains, and practicing mindful eating, you can enjoy festive meals comfortably.
Q6: When should I see a doctor about my diverticulitis diet?
A6: You should consult your GP or a registered dietitian if you have persistent symptoms, concerns about your diet, or need personalized dietary advice. Seek immediate medical attention for severe pain, fever, or bleeding.