Experiencing diverticulitis can be a challenging and often painful journey. Understanding the right dietary approaches is absolutely crucial for managing symptoms, preventing flare-ups, and ultimately, reclaiming your well-being. This comprehensive guide, inspired by the trusted information found in NHS resources, aims to empower you with knowledge about the diverticulitis diet, presented in an accessible and informative way. We’ll explore what the NHS recommends, how to navigate dietary changes, and the vital role of fiber, all while keeping the elusive "diverticulitis diet NHS PDF" in mind.
Understanding Diverticulitis and the Power of Diet
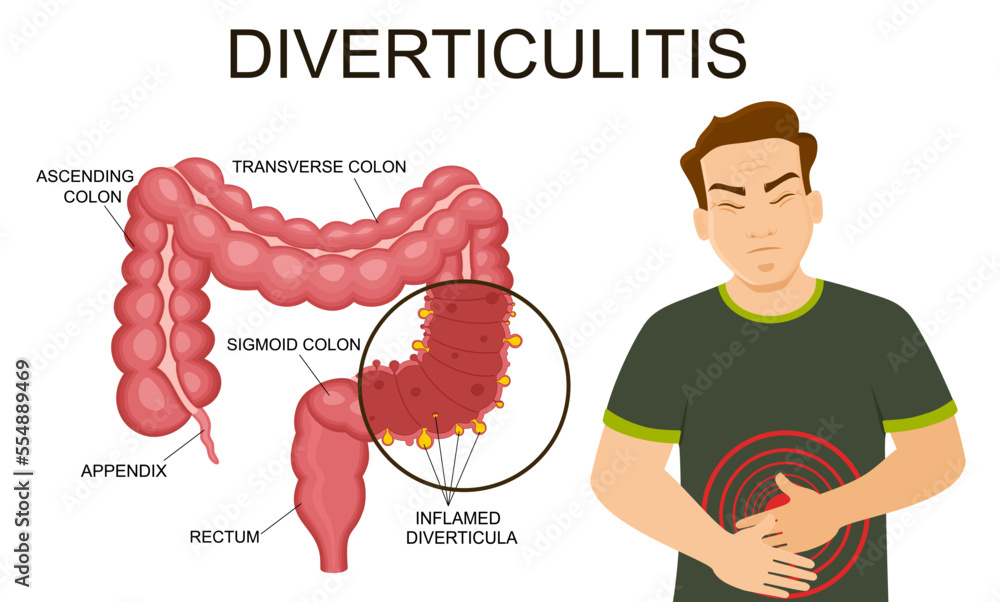
Diverticulitis is a condition that affects the large intestine, specifically the colon. It occurs when small pouches, called diverticula, that form in the wall of the colon become inflamed or infected. While many people have diverticula without experiencing any problems, when these pouches become inflamed, it can lead to significant discomfort, pain, fever, and changes in bowel habits.
The good news is that dietary adjustments play a monumental role in managing diverticulitis. By making informed food choices, you can significantly reduce your risk of developing painful flare-ups and promote a healthier digestive system. This is where the concept of a "diverticulitis diet NHS PDF" becomes so valuable – it represents a reliable source of guidance for those seeking to improve their condition through nutrition.
What is Diverticulitis? A Closer Look
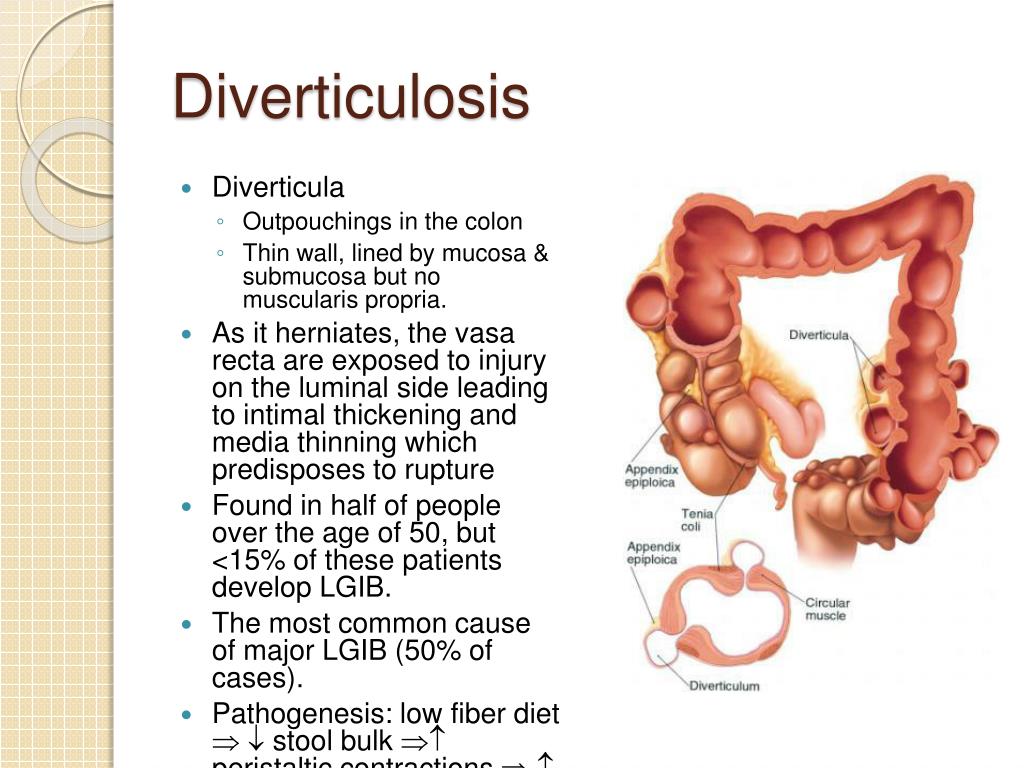
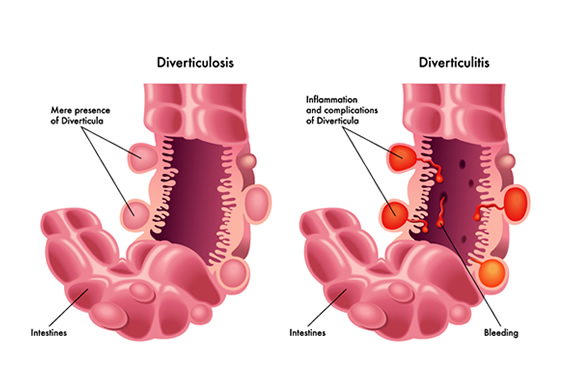
Before diving into dietary specifics, it’s helpful to understand the underlying condition. Diverticula are small, bulging sacs that can form in the lining of your digestive system. They are most common in the lower part of the large intestine (the colon). The presence of these pouches is known as diverticulosis.
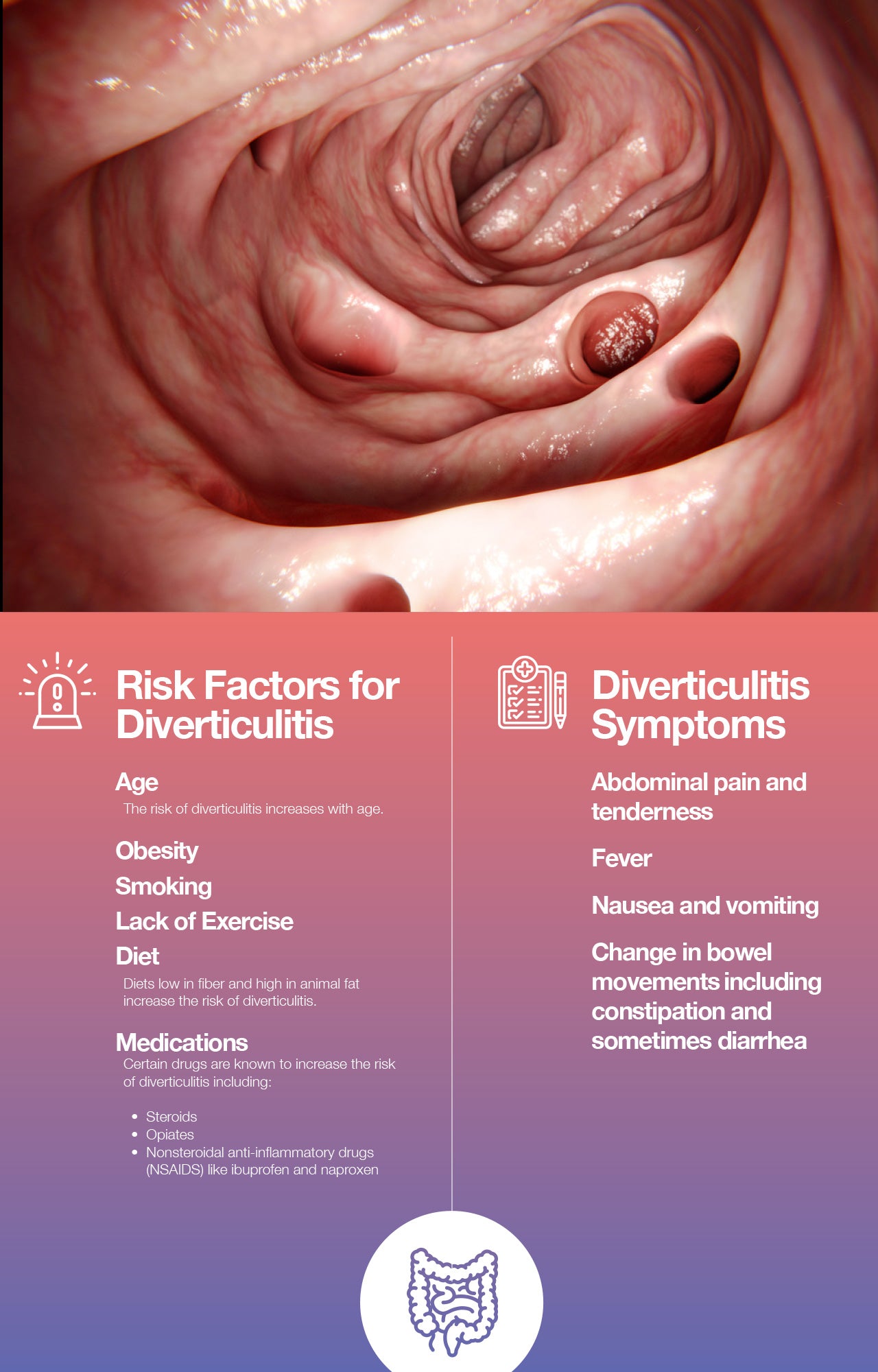
When these pouches become inflamed or infected, the condition is called diverticulitis. This inflammation can cause a range of symptoms, including:
- Abdominal pain: Often on the lower left side, but can occur elsewhere.
- Fever and chills: Indicating an infection.
- Nausea and vomiting: Common responses to inflammation.
- Changes in bowel habits: Constipation or diarrhea.
- Bloating and gas: Due to digestive disruption.
While the exact cause of diverticulitis isn’t always clear, a low-fiber diet is widely believed to be a significant contributing factor to the development of diverticula in the first place.
The Crucial Role of Fiber in Diverticulitis Management
Fiber is a cornerstone of a healthy diet, and its importance is amplified when managing diverticulitis. There are two main types of fiber:
- Soluble fiber: Dissolves in water and forms a gel-like substance. It can help soften stools and regulate blood sugar. Good sources include oats, barley, nuts, seeds, beans, and fruits like apples and citrus.
- Insoluble fiber: Does not dissolve in water and adds bulk to the stool. It helps food pass more quickly through the digestive system. Found in whole grains, vegetables, and wheat bran.
For individuals with diverticulitis, a high-fiber diet is generally recommended to prevent constipation, which can put pressure on the colon and potentially lead to the formation or irritation of diverticula. However, the approach to fiber intake can differ depending on whether you are experiencing an active flare-up or are in remission.
Navigating the Diverticulitis Diet: NHS Guidance and Practical Tips
The National Health Service (NHS) provides invaluable, evidence-based advice on managing various health conditions, including diverticulitis. While a specific, standalone "diverticulitis diet NHS PDF" might not be readily available for direct download in every instance, the principles and recommendations are consistently outlined across their official health information resources. These guidelines are designed to be practical, safe, and effective for the general public.
During a Diverticulitis Flare-Up: A Gentle Approach
When you are experiencing an active diverticulitis flare-up, the primary goal of your diet is to rest your bowel and reduce inflammation. This typically involves a temporary shift to a low-fiber or clear liquid diet.
Clear Liquid Diet: The Initial Step
A clear liquid diet is usually recommended for a short period, typically 2-3 days, or until symptoms begin to improve. This allows your digestive system to rest and recover. Examples of clear liquids include:
- Water
- Clear broths (vegetable or chicken, strained)
- Fruit juices without pulp (apple, grape, cranberry)
- Jell-O (without added fruit pieces)
- Ice pops (without fruit pieces or cream)
- Tea and coffee (without milk or cream)
It’s important to stay well-hydrated during this phase.
Transitioning to a Low-Fiber Diet
As your symptoms improve, you’ll gradually reintroduce solid foods, starting with a low-fiber diet. The aim here is to provide your bowel with easily digestible foods that are less likely to irritate the inflamed areas.
Foods to Include on a Low-Fiber Diet:
- Refined grains: White bread, white rice, plain pasta, refined cereals (like cornflakes or puffed rice).
- Cooked, non-fibrous vegetables: Peeled potatoes, carrots, zucchini (without seeds).
- Fruit juices without pulp: As mentioned above.
- Lean proteins: Well-cooked chicken, turkey, fish, and eggs.
- Dairy products: Milk, yogurt, and cheese (if tolerated).
Foods to Avoid on a Low-Fiber Diet (During a Flare-Up):
- Whole grains
- Nuts and seeds
- Legumes (beans, lentils)
- Raw fruits and vegetables
- Popcorn
- Foods high in fat
- Spicy foods
The transition from a clear liquid to a low-fiber diet should be gradual, with small, frequent meals. Listen to your body and introduce new foods slowly.
Beyond the Flare-Up: Reintroducing Fiber for Long-Term Health
Once the inflammation has subsided and you are symptom-free, the focus shifts to a long-term strategy of gradually increasing your fiber intake. This is crucial for preventing future diverticulitis episodes and promoting overall digestive health. The NHS strongly advocates for a high-fiber diet for long-term prevention.
The Gradual Reintroduction of Fiber
This is a critical phase and requires patience. Suddenly increasing fiber intake can lead to gas, bloating, and discomfort. The key is to do it slowly and consistently.
How to Gradually Increase Fiber:
- Start small: Add one high-fiber food to your diet each day.
- Increase portion sizes slowly: Once you tolerate a new high-fiber food, gradually increase the amount you eat.
- Stay hydrated: Drinking plenty of water is essential for fiber to work effectively and prevent constipation. Aim for at least 8 glasses of water a day.
- Listen to your body: If you experience any discomfort, reduce your fiber intake and try again later.
Excellent Sources of Fiber for Long-Term Management:
- Whole grains: Wholemeal bread, brown rice, oats, quinoa, barley.
- Fruits: Berries, apples (with skin), pears, bananas, prunes.
- Vegetables: Broccoli, Brussels sprouts, spinach, sweet potatoes, carrots.
- Legumes: Lentils, chickpeas, kidney beans, black beans.
- Nuts and seeds: Almonds, walnuts, chia seeds, flaxseeds (in moderation, and ensure good hydration).
Important Note on Nuts, Seeds, and Popcorn: Historically, there was a belief that nuts, seeds, and popcorn could worsen diverticulitis by getting stuck in diverticula. However, current NHS guidance and much of the medical community now suggest that for most people in remission, these foods are generally safe and can be beneficial as part of a high-fiber diet. If you have concerns, discuss them with your doctor or a registered dietitian.
Hydration: The Unsung Hero of a Diverticulitis Diet
Adequate fluid intake is paramount for everyone, but it’s especially vital when managing diverticulitis. Water helps to soften stools, making them easier to pass and reducing the strain on your colon. It also aids in the effective functioning of fiber in your digestive system.
- Aim for at least 1.5 to 2 liters of fluid per day.
- Water is the best choice.
- Other good options include: herbal teas, clear broths, and diluted fruit juices.
- Limit sugary drinks and excessive caffeine, as they can be dehydrating for some individuals.
Beyond Diet: Lifestyle Factors for Diverticulitis Management
While diet is a powerful tool, a holistic approach to managing diverticulitis also involves considering other lifestyle factors.
Regular Exercise: A Gentle Boost for Digestion
Engaging in regular physical activity can help stimulate bowel function and promote overall digestive health. Aim for moderate exercise most days of the week.
Stress Management: The Gut-Brain Connection
Stress can significantly impact your digestive system. Finding healthy ways to manage stress, such as mindfulness, yoga, or spending time in nature, can be beneficial.
Avoiding Smoking: A Known Risk Factor
Smoking is detrimental to overall health and can exacerbate inflammatory conditions, including diverticulitis. Quitting smoking is one of the best things you can do for your well-being.
Finding Reliable Information: The "Diverticulitis Diet NHS PDF" Quest
Many individuals search for a specific "diverticulitis diet NHS PDF" to have a tangible, printable guide. While a single, universally downloadable PDF might not always be directly linked, the NHS website is an excellent and authoritative resource. You can find detailed information on diverticulitis and dietary recommendations by searching their site for "diverticulitis" or "diet and digestive health." Often, these pages will contain links to downloadable leaflets or provide comprehensive information that can be printed.
Key takeaway: Trustworthy information regarding the diverticulitis diet is readily available through official NHS channels. Focus on understanding the principles rather than solely on finding a specific PDF.
Frequently Asked Questions About the Diverticulitis Diet
Here are some common questions people have about managing diverticulitis through diet:
Q1: What is the most important dietary change for diverticulitis?
A1: The most crucial dietary change is managing your fiber intake. During a flare-up, a low-fiber diet is recommended, and for long-term prevention, a gradual increase to a high-fiber diet is essential.
Q2: Can I eat nuts and seeds with diverticulitis?
A2: For most people in remission, nuts and seeds are safe and can be beneficial as part of a high-fiber diet. If you have concerns or have experienced issues in the past, discuss this with your doctor.
Q3: How long should I follow a clear liquid diet during a flare-up?
A3: A clear liquid diet is typically followed for a short period, usually 2-3 days, or until Calorie low carb diet plan australia your ultimate guide to amazing results your symptoms start to improve. Your doctor will advise you on when to transition to other foods.
Q4: What are the best foods to eat to prevent diverticulitis?
A4: A long-term high-fiber diet rich in whole grains, fruits, vegetables, and legumes is recommended for preventing diverticulitis. Staying well-hydrated is also crucial.
Q5: Should I avoid red meat if I have diverticulitis?
A5: While a high-fiber diet is key, some studies suggest that diets high in red meat and low in fiber may be associated with an increased risk of diverticulitis. Focusing on lean proteins and a balanced, high-fiber diet is generally advised.
Conclusion: Empowering Your Digestive Health Journey
Managing diverticulitis is a journey that often involves significant dietary adjustments. By understanding the principles of a diverticulitis diet, as guided by trusted sources like the NHS, you can take proactive steps towards managing your condition, reducing the risk of flare-ups, and improving your overall digestive well-being. Remember, patience, consistency, and listening to your body are your greatest allies. If you are struggling to find specific NHS resources or have concerns about your diet, always consult with your doctor or a registered dietitian. They can provide personalized advice tailored to your individual needs and medical history. Share this information with others who might benefit from a clearer understanding of the diverticulitis diet NHS PDF and the path to digestive comfort!