The festive season often brings joy, family, and an abundance of delicious food. However, for those managing diverticulitis, navigating holiday feasts can feel like a minefield. Understanding the right diverticulitis diet recommendations NHS provides is crucial for enjoying this time of year without the unwelcome disruption of flare-ups. This comprehensive guide, inspired by the trusted advice from the NHS, aims to illuminate the path to a comfortable and joyous holiday for everyone.
Understanding Diverticulitis: A Gentle Explanation
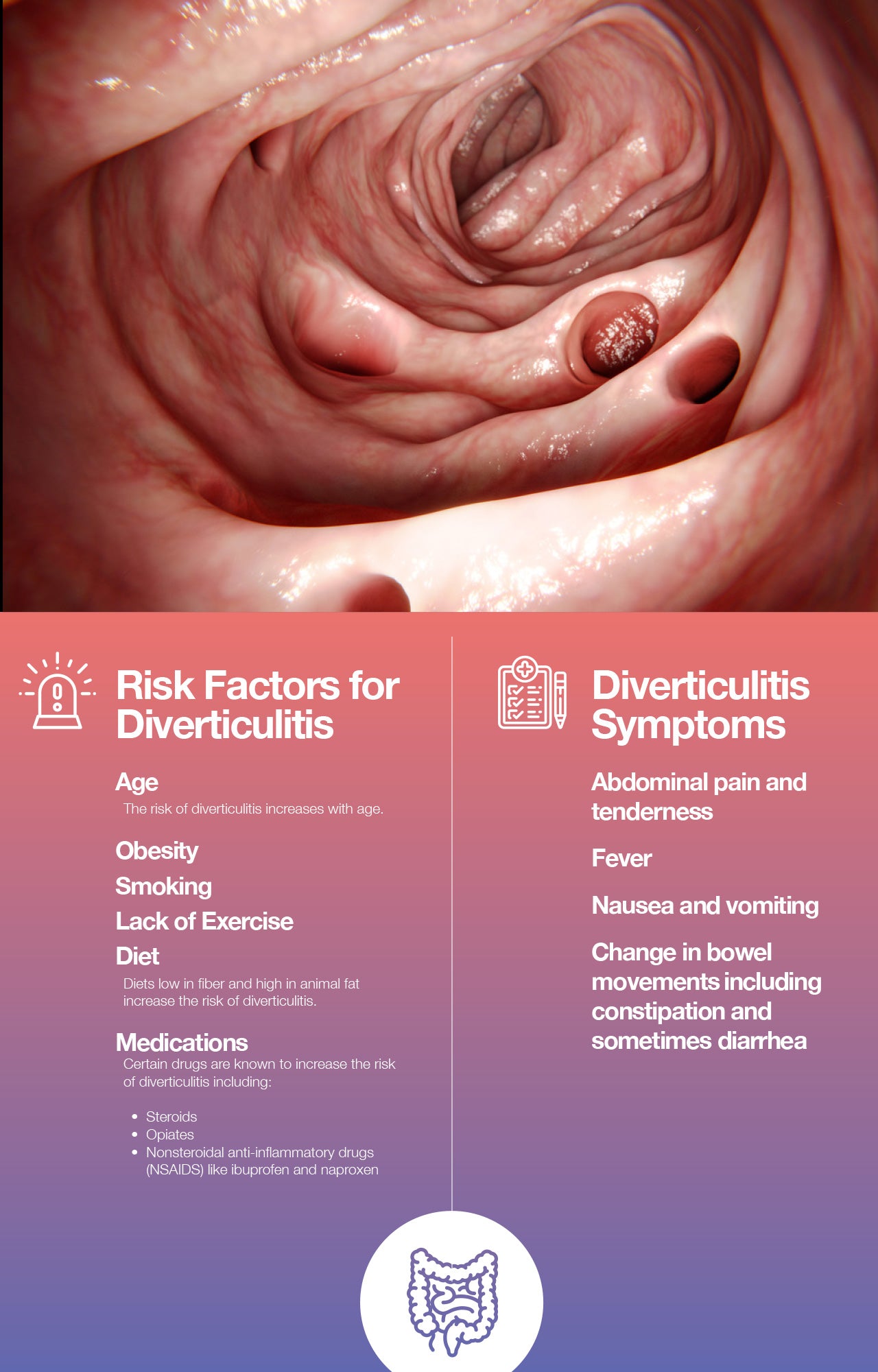
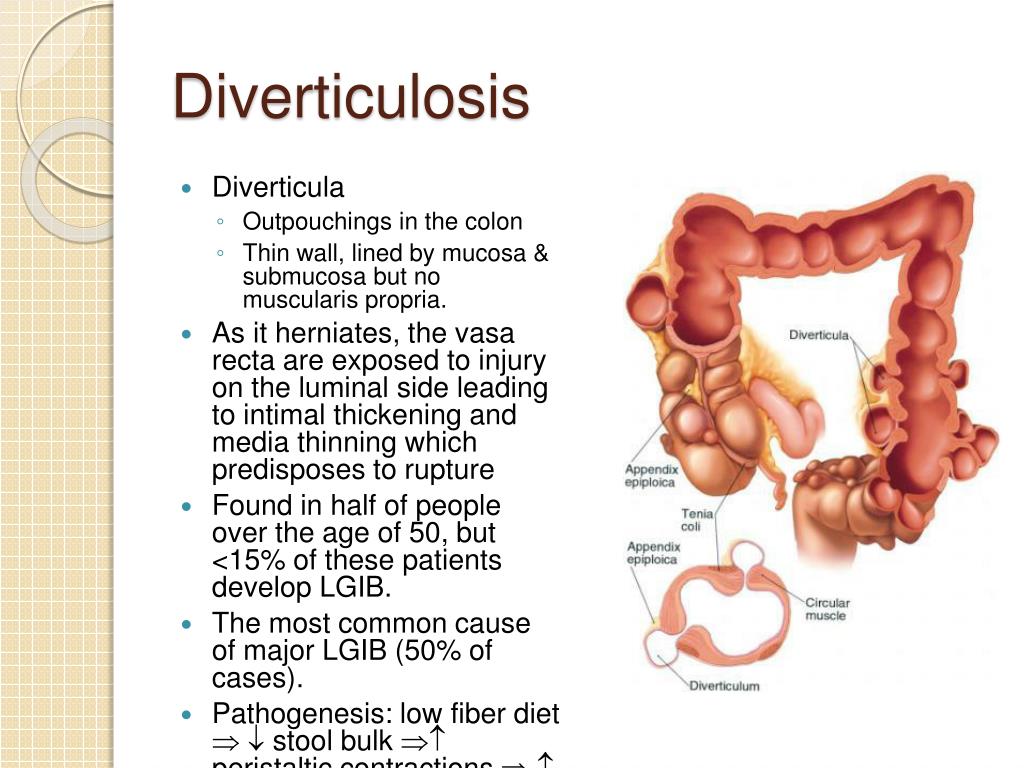
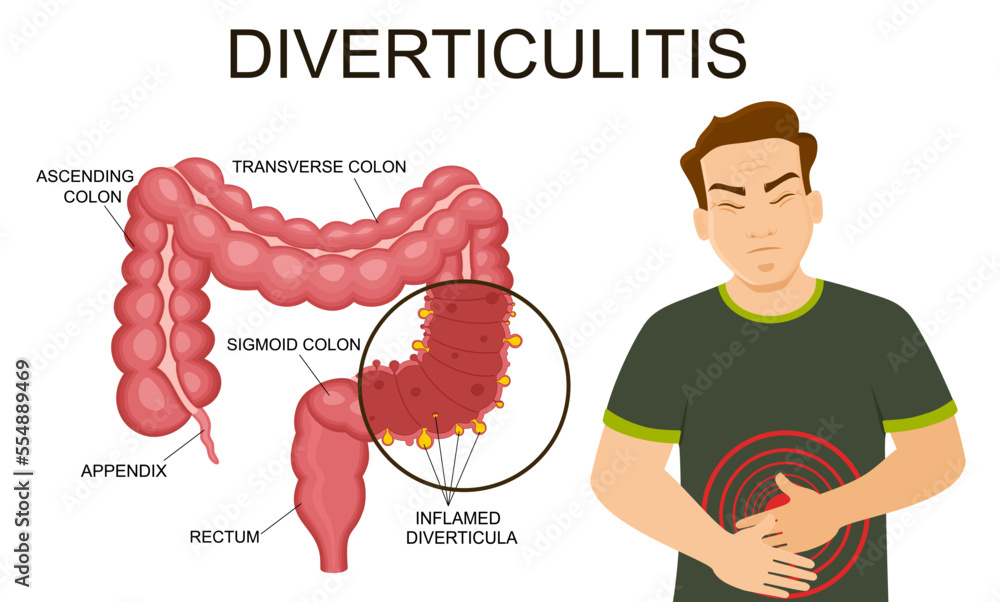
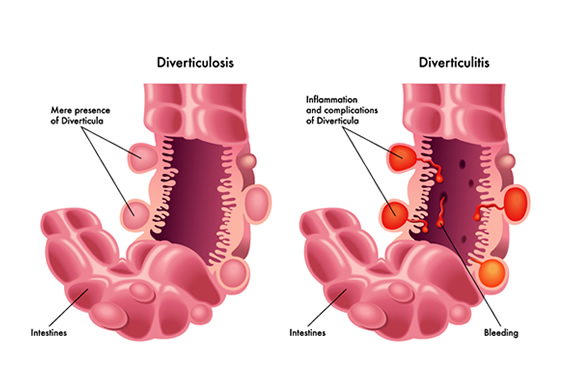
Before diving into dietary recommendations, let’s briefly touch upon what diverticulitis is. Diverticula are small, bulging pouches that can form in the lining of your digestive system, most commonly in the large intestine (colon). When these pouches become inflamed or infected, it’s known as diverticulitis. While the exact cause isn’t always clear, a low-fibre diet is often implicated in the development of diverticular disease, and certain foods can trigger symptoms during a flare-up.
Navigating the NHS Diverticulitis Diet: A Two-Phase Approach
The NHS generally recommends a two-phase approach to managing diverticulitis through diet: an initial phase for managing acute flare-ups and a long-term phase for prevention and ongoing gut health.
Phase 1: Managing Acute Diverticulitis Flare-Ups
During an active diverticulitis flare-up, your digestive system needs a rest. The primary goal is to reduce inflammation and allow the bowel to heal. This typically involves a temporary shift to a low-fibre, or clear liquid, diet.
Clear Liquid Diet: The Initial Step
A clear liquid diet is designed to be easily digestible and leave minimal residue in the bowel. Think of it as giving your gut a much-needed break. Examples of clear liquids include:
- Water: Plain, sparkling, or with a squeeze of lemon or lime.
- Clear broths: Chicken, beef, or vegetable broth (strained to remove any solids).
- Fruit juices without pulp: Apple juice, grape juice, cranberry juice.
- Jellies (gelatin desserts): Plain flavours like lemon, lime, or apple.
- Ice pops: Made from clear fruit juices.
- Tea and coffee: Without milk or cream.
It’s important to stay well-hydrated during this phase. Aim to sip fluids throughout the day. The duration of a clear liquid diet will vary depending on the severity of the flare-up and your doctor’s advice.
Transitioning to a Low-Fibre Diet
Once your symptoms begin to improve, you’ll gradually transition to a low-fibre diet. This means choosing foods that are easily digested and produce less bulk in your stool. The aim is to continue reducing the strain on your inflamed bowel.
Foods to Embrace on a Low-Fibre Diet:
- Refined grains: White bread, white rice, plain pasta, cream of wheat, cornflakes.
- Cooked, seedless, and skinless fruits: Applesauce, peeled pears, canned peaches (without skin).
- Cooked, seedless, and skinless vegetables: Well-cooked carrots, potatoes (peeled), spinach (well-cooked).
- Lean proteins: Plain chicken or turkey (skinless), fish, eggs, tofu.
- Dairy products (if tolerated): Milk, yogurt, cheese.
Foods to Temporarily Avoid on a Low-Fibre Diet:
- Whole grains: Wholemeal bread, brown rice, oats, quinoa.
- Raw fruits and vegetables: Especially those with skins and seeds.
- Legumes: Beans, lentils, peas.
- Nuts and seeds.
- Spicy foods.
- Fatty or fried foods.
- Alcohol.
The transition from a clear liquid diet to a low-fibre diet should be gradual. Introduce new foods one at a time to see how your body reacts. Listen to your body – if a particular food causes discomfort, stop eating it and consult your doctor.
Phase 2: Long-Term Management and Prevention
Once the flare-up has subsided and you’re feeling better, the focus shifts to a long-term diet that promotes gut health and helps prevent future diverticulitis episodes. This is where the emphasis on diverticulitis diet recommendations NHS truly shines, advocating for a high-fibre diet.
The Power of Fibre: Your Gut’s Best Friend
Contrary to what you might think during a flare-up, fibre is essential for preventing diverticulitis in the long run. A high-fibre diet helps to keep your bowel movements regular and soft, reducing pressure within the colon. This, in turn, can prevent the formation of new diverticula and reduce the risk of inflammation in existing ones.
Gradually Increasing Fibre Intake:
It’s crucial to increase your fibre intake gradually to avoid gas, bloating, and discomfort. A sudden jump in fibre can overwhelm your digestive system. Aim to add one high-fibre food to your diet every few days.
Excellent Sources of Fibre:
- Fruits: Berries, apples (with skin), pears (with skin), bananas, oranges.
- Vegetables: Broccoli, Brussels sprouts, carrots, sweet potatoes, leafy greens (kale, spinach).
- Whole grains: Wholemeal bread, brown rice, oats, barley, quinoa, wholewheat pasta.
- Legumes: Lentils, chickpeas, kidney beans, black beans.
- Nuts and seeds: Almonds, walnuts, chia seeds, flaxseeds.
Hydration is Weight loss for year old girls a healthy happy journey Key with Fibre:
When increasing your fibre intake, it’s absolutely vital to drink plenty of water. Fibre absorbs water, and without adequate hydration, it can lead to constipation, which is counterproductive. Aim for at least 8 glasses of water a day, and more if you’re physically active or in a warm climate.
Foods to Continue Limiting (Even in Long-Term Management)
While the focus shifts to high fibre, some foods may still be best enjoyed in moderation or avoided altogether, depending on individual tolerance.
- Red meat: Can be harder to digest for some.
- Processed foods: Often low in fibre and high in unhealthy fats and sugars.
- Spicy foods: Can irritate the digestive system.
- Alcohol: Can dehydrate and irritate the gut.
- Fatty and fried foods: Can be difficult to digest.
The Nuts and Seeds Debate:
Historically, there was a belief that nuts and seeds could get stuck in diverticula and cause inflammation. However, current NHS guidance and most medical professionals now agree that nuts and seeds are generally safe and beneficial for most people with diverticular disease, as they are excellent sources of fibre. If you find they cause you discomfort, you can discuss this with your doctor.
Practical Tips for a Festive and Gut-Friendly Holiday
Navigating the festive season with diverticulitis doesn’t mean missing out on the joy. Here are some practical tips to help you enjoy the celebrations while being mindful of your gut health:
- Plan Ahead: Before attending any gatherings, think about the food that will be served. If possible, have a light, safe meal before you go to avoid arriving ravenous and tempted by everything.
- Portion Control: Even with safe foods, moderation is key. Enjoy small portions of everything you choose.
- Listen to Your Body: This is the most important rule. If a food doesn’t feel right, don’t eat it. Pay attention to how your body reacts to different foods.
- Stay Hydrated: Keep a water bottle with you and sip throughout the day. This is especially important during festive meals when you might be consuming more sodium.
- Choose Wisely: Opt for lean proteins, cooked vegetables, and whole grains where available. Be cautious with rich sauces, creamy dishes, and fried foods.
- Communicate (If Comfortable): If you feel comfortable, you can let your host know about your dietary needs. Most people are understanding and happy to accommodate.
- Enjoy the Company: Remember that the festive season is about more than just food. Focus on connecting with loved ones and enjoying the atmosphere.
- Post-Festive Recovery: If you do overindulge or experience mild discomfort, return to your prescribed diet immediately and ensure you’re drinking plenty of fluids.
When to Seek Medical Advice
It’s essential to consult your doctor or a registered dietitian for personalized diverticulitis diet recommendations NHS provides. They can assess your individual needs, medical history, and current condition to offer the most appropriate dietary advice.
Seek immediate medical attention if you experience:
- Severe abdominal pain.
- Fever.
- Chills.
- Nausea and vomiting.
- Blood in your stool.
These could be signs of a more serious complication of diverticulitis.
Frequently Asked Questions About Diverticulitis Diet
Q1: Can I eat popcorn with diverticulitis?
While the old advice was to avoid popcorn, current thinking suggests that if you tolerate it well and it doesn’t cause you discomfort, it can be a good source of fibre. However, if you’ve had issues in the past, it’s best to err on the side of caution or discuss it with your doctor.
Q2: Is a low-fibre diet permanent for diverticulitis?
No, a low-fibre diet is typically a temporary measure for managing acute flare-ups. The long-term goal, as recommended by the NHS, is to gradually increase fibre intake to promote gut health and prevent future episodes.
Q3: What are the best drinks for diverticulitis?
During a flare-up, clear liquids like water, clear broths, and pulp-free juices are best. For long-term management, water is paramount, especially when increasing fibre intake. Other beneficial drinks include herbal teas.
Q4: Can I eat spicy food with diverticulitis?
Spicy foods can be a trigger for diverticulitis symptoms in some individuals. It’s generally advisable to limit or avoid spicy foods, especially during a flare-up and when transitioning to a high-fibre diet.
Q5: How much fibre should I aim for daily with diverticulitis?
The recommended daily fibre intake for adults is generally around 30 grams. However, it’s crucial to increase this gradually and under the guidance of a healthcare professional to avoid digestive upset.
Conclusion: Embracing a Healthier Gut for Happier Holidays
Navigating diverticulitis diet recommendations NHS provides can empower you to enjoy the festive season and beyond with greater comfort and confidence. By understanding the phases of dietary management – from the initial rest during a flare-up to the long-term benefits of a high-fibre diet – you can make informed choices that support your gut health. Remember, this is a journey, and with the right knowledge and support, you can continue to celebrate life’s joys without the worry of diverticulitis holding you back. Share this guide with friends and family who might benefit, and let’s all aim for a healthier, happier gut this holiday season!