Feeling bloated, uncomfortable, or experiencing sharp abdominal pain? You might be dealing with diverticulitis, a common condition affecting the large intestine. But don’t despair! Understanding the right diet is your most powerful weapon in managing this condition and reclaiming your digestive comfort. This comprehensive diverticulitis diet education handout is designed to empower you with the knowledge you need to navigate your meals with confidence and celebrate a happier, healthier gut.
Understanding Diverticulitis: A Gentle Introduction
Before we dive into the specifics of dietary management, let’s briefly touch upon what diverticulitis is. The colon, or large intestine, is a muscular tube that absorbs water and electrolytes from digested food and then passes the remaining waste material out of the body. In some individuals, small, bulging pouches called diverticula can form in the colon wall. When these pouches become inflamed or infected, it’s known as diverticulitis. This can lead to a range of symptoms, from mild discomfort to severe pain, fever, and changes in bowel habits.
While diverticulitis can be a challenging condition, the good news is that with the right approach, many people can significantly reduce the frequency and severity of flare-ups. A well-informed diet plays a pivotal role in this journey, acting as a gentle yet effective guide towards digestive well-being.
The Crucial Role of Diet in Diverticulitis Management
Your diet is more than just sustenance; it’s a powerful tool that can either aggravate or soothe your digestive system. For individuals with diverticulitis, making informed food choices is paramount. This diverticulitis diet education handout aims to demystify the dietary recommendations, providing clear, actionable advice to help you feel your best. We’ll explore the phases of dietary management, focusing on what to eat and what to avoid during both active flare-ups and periods of remission.
Navigating a Diverticulitis Flare-Up: The Initial Steps
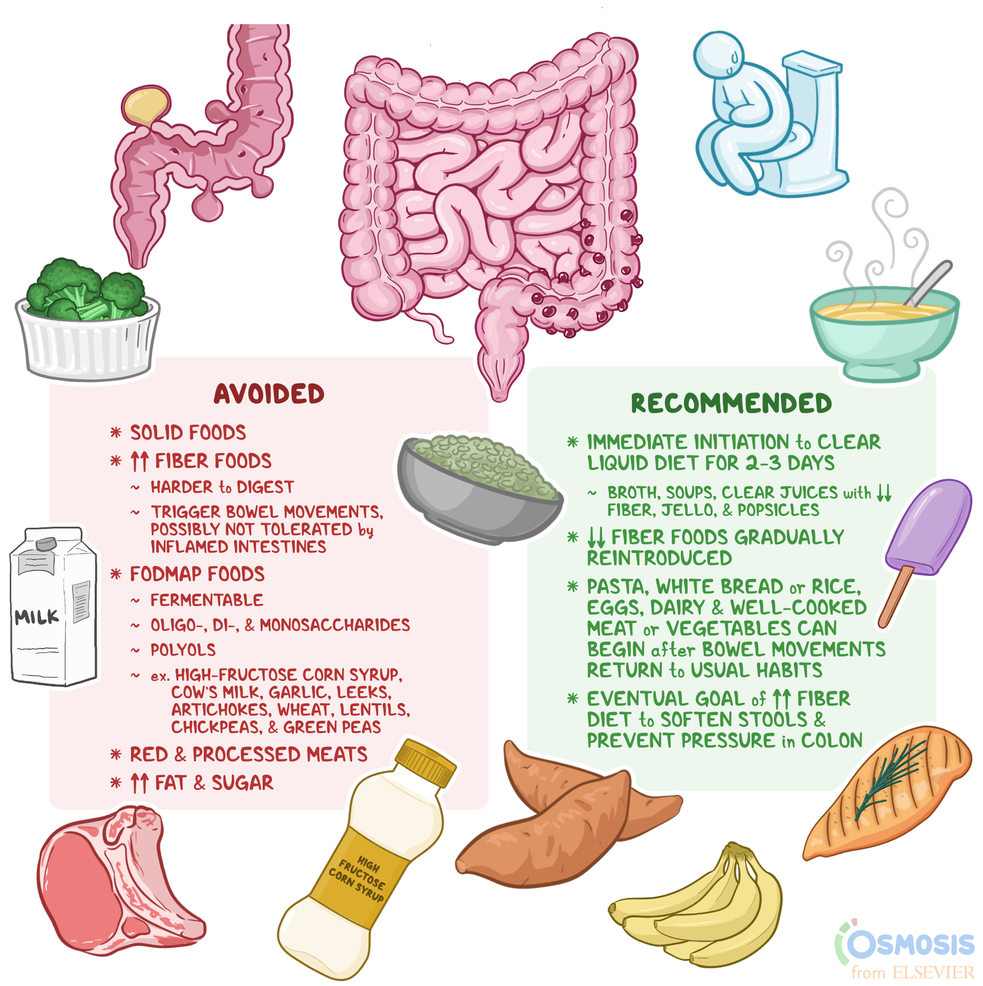
When you’re experiencing an active diverticulitis flare-up, the primary goal is to give your inflamed colon a much-needed rest. This often involves a temporary shift to a clear liquid diet or a low-fiber diet. The idea is to minimize the amount of undigested material passing through your colon, thereby reducing irritation and inflammation.
The Clear Liquid Diet: A Temporary Respite
A clear liquid diet consists of liquids that you can see through. This phase is typically short-term, lasting only a few days until symptoms begin to improve.
-
What to Enjoy:
- Water (plain, carbonated, or flavored without pulp)
- Clear broths (chicken, beef, or vegetable)
- Fruit juices without pulp (apple, white grape, cranberry)
- Gelatin (Jell-O) in clear colors
- Popsicles (without fruit pieces or pulp)
- Tea and coffee (without milk or cream)
-
What to Avoid:
- Milk and dairy products
- Juices with pulp
- Smoothies
- Soups with solid ingredients
- Alcoholic beverages
Transitioning to a Low-Fiber Diet: Gradually Reintroducing Solids
As your symptoms subside, you’ll gradually transition to a low-fiber diet. The aim here is to introduce easily digestible foods that produce less bulk in your stool. This phase is crucial for a smooth recovery and should be guided by your healthcare provider.
-
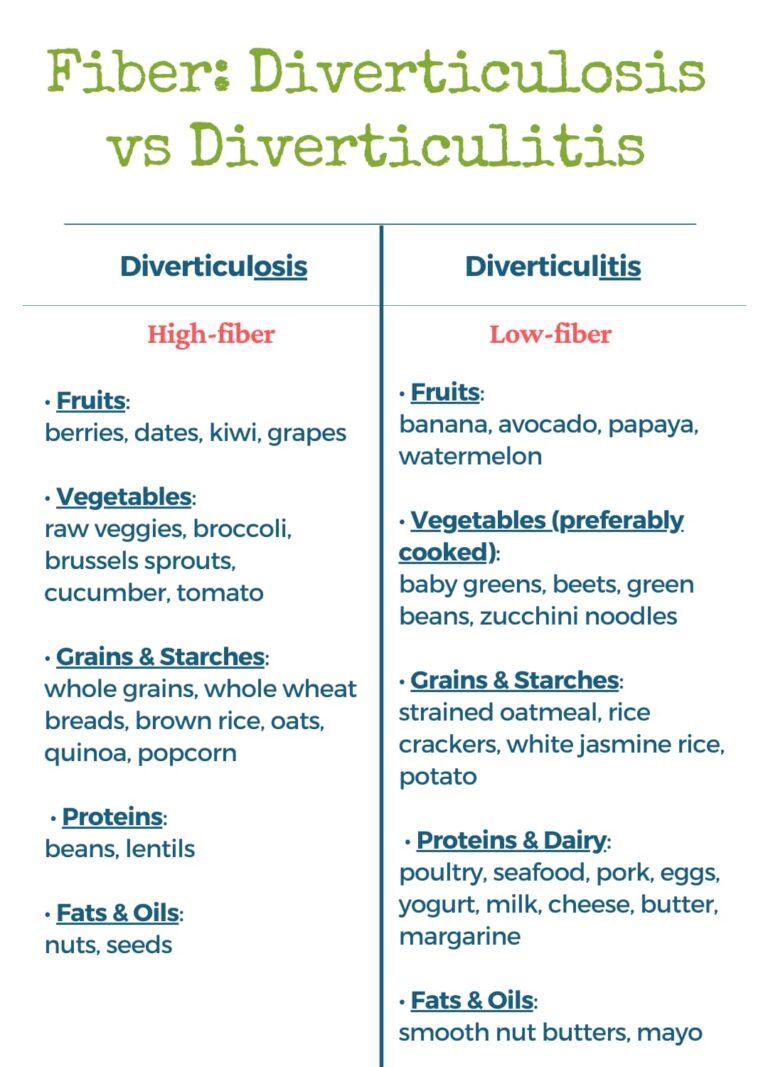
What to Embrace (Low-Fiber Options):
- Refined Grains: White bread, white rice, pasta made from refined flour, plain crackers.
- Cooked Vegetables (peeled and seedless): Well-cooked carrots, green beans, potatoes (without skin), asparagus tips.
- Fruits (peeled and seedless): Applesauce, canned peaches or pears (without skin), ripe bananas.
- Lean Proteins: Skinless chicken or turkey, fish, eggs, tofu.
- Dairy (if tolerated): Milk, yogurt, cheese (low-lactose options may be better for some).
-
What to Temporarily Limit or Avoid (High-Fiber Foods):
- Whole grains (whole wheat bread, brown rice, oats)
- Raw vegetables and fruits with skins and seeds
- Legumes (beans, lentils, peas)
- Nuts and seeds
- Popcorn
Rebuilding Your Gut Health: The Long-Term Diverticulitis Diet
Once you’re symptom-free, the focus shifts to a long-term Diet plans where food is delivered for health a joyful revolution in wellness dietary strategy aimed at preventing future flare-ups and promoting overall gut health. This is where the concept of high-fiber diet for diverticulitis becomes essential. Contrary to what some might believe, a high-fiber diet is generally recommended for preventing diverticulitis in the long run. Fiber helps to keep your stools soft and bulky, reducing pressure in the colon and making it less likely for diverticula to become inflamed.
Embracing a High-Fiber Diet: Your Path to Prevention
The key to a successful high-fiber diet is to introduce fiber gradually to avoid gas and bloating. Aim for a variety of fiber-rich foods to ensure you’re getting a broad spectrum of nutrients.
-
Whole Grains:
- Whole wheat bread and pasta
- Brown rice
- Oats and oatmeal
- Quinoa
- Barley
-
Fruits (with skin and seeds where appropriate):
- Berries (raspberries, blueberries, strawberries)
- Apples and pears (with skin)
- Oranges and other citrus fruits
- Prunes
-
Vegetables (all types, including raw and cooked):
- Broccoli
- Brussels sprouts
- Spinach and kale
- Sweet potatoes
- Artichokes
-
Legumes:
- Beans (black beans, kidney beans, chickpeas)
- Lentils
- Peas
-
Nuts and Seeds:
- Almonds
- Walnuts
- Chia seeds
- Flaxseeds
Important Note on Nuts, Seeds, and Popcorn: For many years, it was believed that nuts, seeds, and popcorn should be avoided due to the concern that they could get lodged in diverticula and cause inflammation. However, current research suggests that for most people, these foods are safe and beneficial as part of a high-fiber diet. If you have experienced issues with these foods in the past, discuss them with your doctor or a registered dietitian.
Hydration: The Unsung Hero of Digestive Health
Adequate fluid intake is crucial for fiber to work effectively. Water helps to soften stools and prevent constipation, which can be a trigger for diverticulitis.
- Aim for: At least 8 glasses (64 ounces) of water per day.
- Other good sources: Herbal teas, clear broths, and water-rich fruits and vegetables.
- Limit: Sugary drinks, excessive caffeine, and alcohol, as they can be dehydrating.
Foods to Approach with Caution (Individual Tolerance Varies)
While a high-fiber diet is generally beneficial, some individuals may find that certain foods trigger their diverticulitis symptoms, even during remission. It’s essential to listen to your body and identify your personal triggers.
- Spicy Foods: Some people find that very spicy foods can irritate their digestive system.
- Fatty and Fried Foods: These can be harder to digest and may contribute to discomfort.
- Red Meat: While not universally problematic, some individuals find that reducing red meat intake helps.
- Processed Foods: These are often low in fiber and high in unhealthy fats and additives.
Creating Your Personalized Diverticulitis Diet Plan
This diverticulitis diet education handout provides general guidelines. However, the most effective approach is to create a personalized plan in collaboration with your healthcare provider or a registered dietitian. They can help you:
- Assess your individual needs and tolerances.
- Develop a gradual plan for increasing fiber intake.
- Identify specific trigger foods.
- Ensure you’re meeting all your nutritional requirements.
Lifestyle Factors Beyond Diet
While diet is a cornerstone of diverticulitis management, other lifestyle factors also play a significant role.
- Regular Exercise: Physical activity promotes bowel regularity and can help reduce the risk of diverticulitis. Aim for at least 30 minutes of moderate-intensity exercise most days of the week.
- Stress Management: Chronic stress can negatively impact digestive health. Incorporate stress-reducing activities like yoga, meditation, or deep breathing exercises into your routine.
- Adequate Sleep: Getting enough quality sleep is vital for overall health, including digestive function.
When to Seek Medical Advice
This diverticulitis diet education handout is for informational purposes only and should not replace professional medical advice. It’s crucial to consult your doctor if you:
- Experience severe abdominal pain.
- Develop a fever.
- Notice significant changes in your bowel habits (persistent constipation or diarrhea).
- See blood in your stool.
- Have any concerns about your diet or symptoms.
Celebrating Your Digestive Wellness Journey
Managing diverticulitis is a journey, and this diverticulitis diet education handout is your companion. By understanding the principles of dietary management and working closely with your healthcare team, you can significantly improve your quality of life. Embrace the power of a balanced, fiber-rich diet, stay hydrated, and remember to listen to your body. With informed choices and a proactive approach, you can navigate diverticulitis with confidence and celebrate the joy of a healthy, happy digestive system.
Frequently Asked Questions (FAQ)
Q1: What is the main goal of a diverticulitis diet?
A1: The main goal is to reduce inflammation and discomfort during a flare-up and to prevent future flare-ups by promoting regular bowel movements and reducing pressure in the colon.
Q2: Should I avoid all fiber if I have diverticulitis?
A2: During an active flare-up, a temporary low-fiber or clear liquid diet is recommended. However, for long-term management and prevention, a high-fiber diet is generally advised.
Q3: Are nuts and seeds safe to eat with diverticulitis?
A3: For most people, nuts, seeds, and popcorn are safe and beneficial as part of a high-fiber diet. If you’ve had issues with them in the past, discuss this with your doctor.
Q4: How much water should I drink daily for diverticulitis?
A4: Aim for at least 8 glasses (64 ounces) of water per day to help fiber work effectively and prevent constipation.
Q5: Can I eat spicy foods with diverticulitis?
A5: Some individuals find that spicy foods can trigger symptoms. It’s best to monitor your own tolerance and discuss with your doctor if you have concerns.
Q6: How quickly can I return to a normal diet after a diverticulitis flare-up?
A6: The transition from a liquid or low-fiber diet back to a regular diet should be gradual and guided by your healthcare provider, typically over several days to a week as symptoms improve.