Experiencing diverticulitis can be a challenging journey, but understanding your diet is your powerful ally in managing symptoms and preventing future flare-ups. This comprehensive diverticulitis diet handout for patients is designed to be your go-to resource, offering clear, actionable advice to help you navigate your dietary choices with confidence. We’re here to illuminate the path towards a more comfortable and vibrant you, transforming dietary concerns into a celebration of well-being!
Understanding Diverticulitis and the Role of Diet
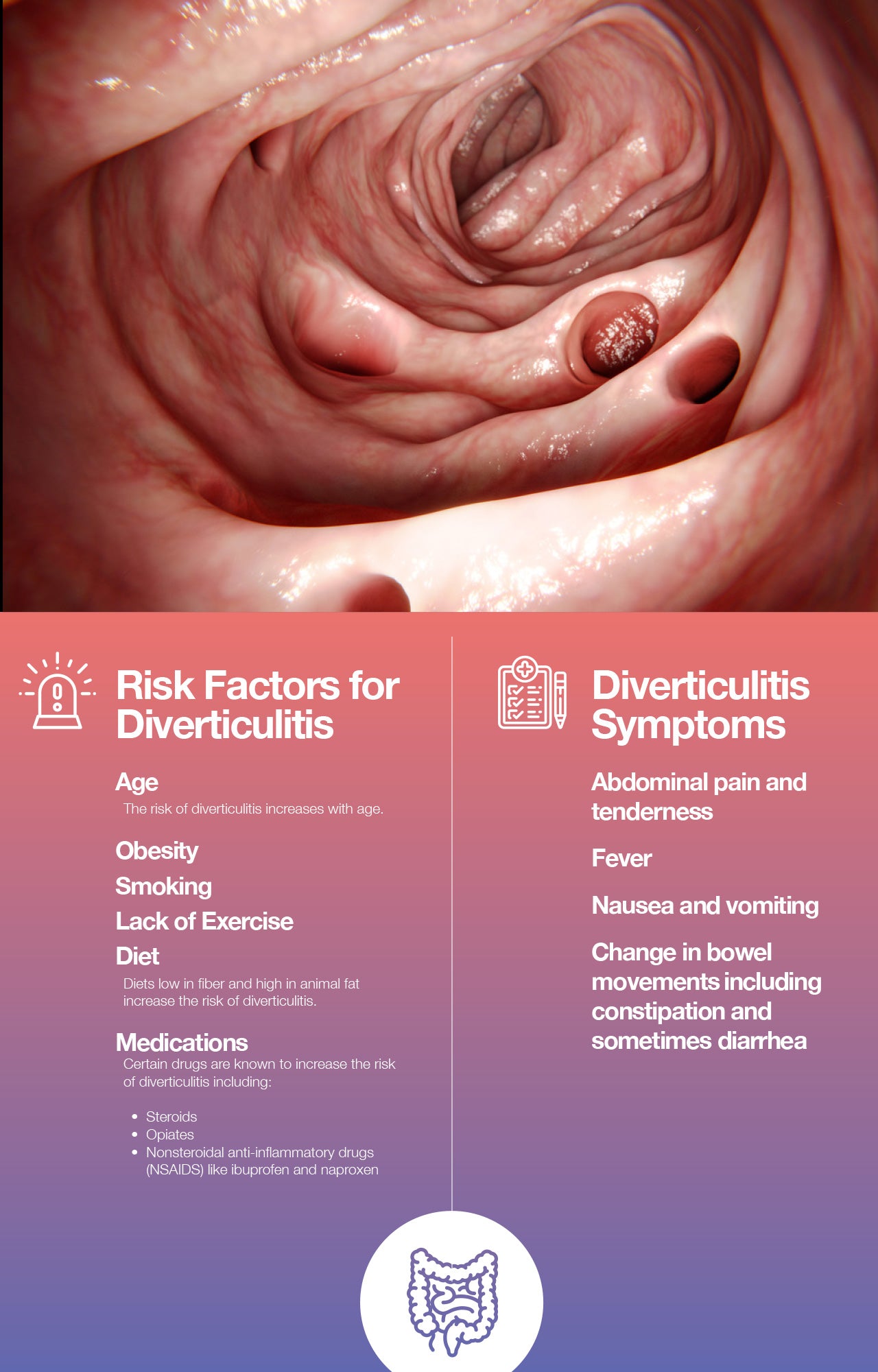
Diverticulitis occurs when small pouches, called diverticula, that form in the wall of your colon become inflamed or infected. While the exact cause isn’t always clear, dietary factors are strongly implicated in both the development and management of this condition. A well-structured diet can significantly reduce the risk of diverticulitis attacks and alleviate the discomfort associated with them.
What are Diverticula and Diverticulitis?
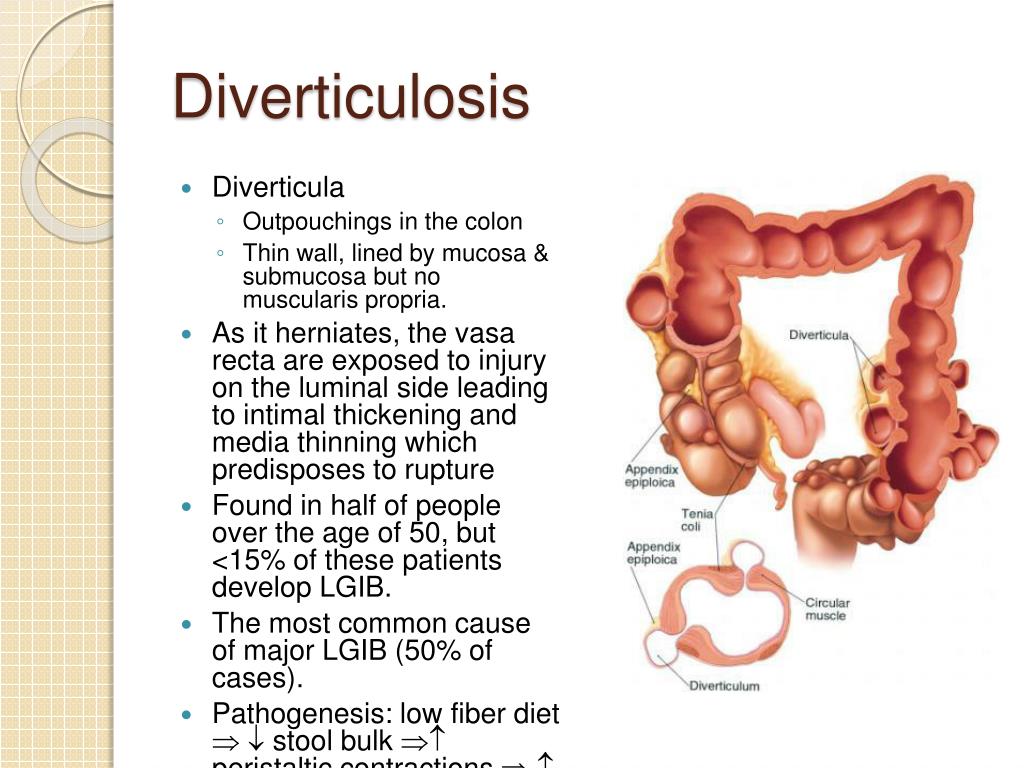
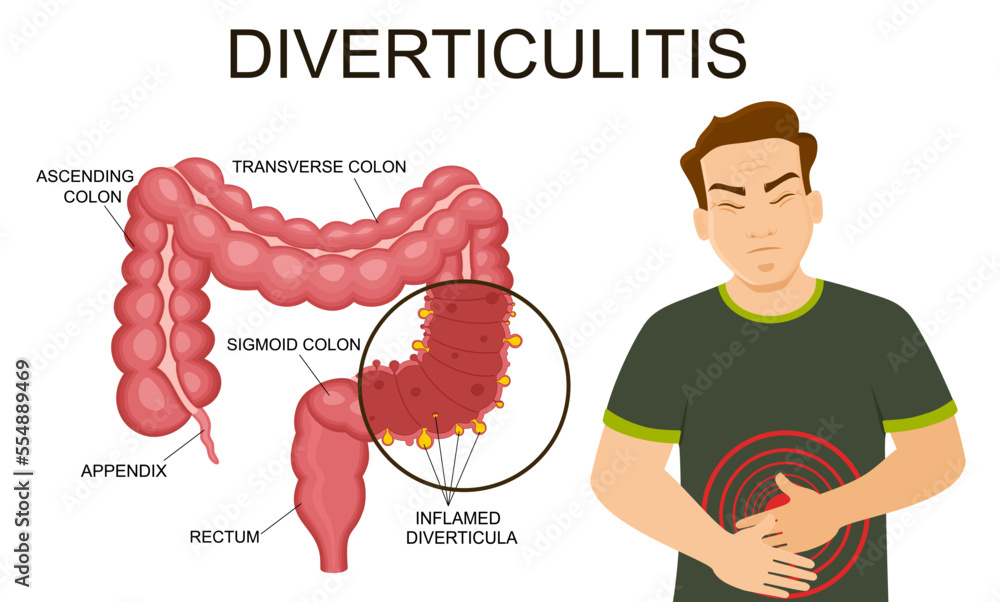
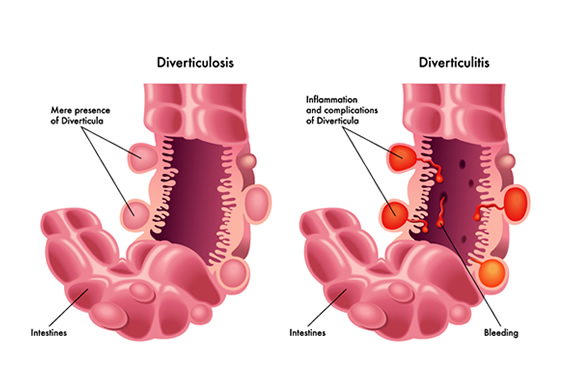
Diverticula are tiny, sac-like protrusions that can develop in the lining of the digestive tract, most commonly in the large intestine (colon). They are often asymptomatic and quite common, especially as people age. Diverticulosis refers to the presence of these pouches. Diverticulitis, on the other hand, is the inflammation or infection of these diverticula, leading to symptoms like abdominal pain, fever, nausea, and changes in bowel habits.
The Crucial Link Between Diet and Diverticulitis
For decades, medical professionals have recognized the profound impact of diet on diverticular health. A low-fiber diet has long been suspected as a primary contributor to the formation of diverticula. Conversely, a high-fiber diet is considered a cornerstone of prevention and management for diverticulitis. This diverticulitis diet handout for patients emphasizes how specific food choices can either soothe your digestive system or inadvertently trigger discomfort.
Navigating the Phases: Acute vs. Chronic Diverticulitis Diet
The dietary recommendations for diverticulitis often change depending on whether you are experiencing an acute flare-up or are in a period of remission. This section of our diverticulitis diet handout for patients will guide you through these distinct phases.
During an Acute Diverticulitis Flare-Up: The Clear Liquid Diet
When diverticulitis is active and causing significant pain and inflammation, your doctor will likely recommend a temporary clear liquid diet. The goal here is to give your digestive system a much-needed rest.
Foods and Drinks to Embrace (Clear Liquid Phase):
- Water: Plain, sparkling, or infused with a hint of lemon or lime.
- Broth: Clear chicken, beef, or vegetable broth (strained to remove any solids).
- Juices: Strained apple juice, white grape juice, or cranberry juice (without pulp).
- Gelatin: Plain gelatin desserts (like Jell-O) in clear colors.
- Popsicles: Made from clear juices, without fruit pieces or dairy.
- Tea and Coffee: Without milk, cream, or artificial sweeteners (though some may prefer to avoid caffeine during a flare).
Foods and Drinks to Strictly Avoid (Clear Liquid Phase):
- Anything with pulp or solid particles.
- Milk and dairy products.
- Juices with pulp.
- Alcoholic beverages.
- Sugary drinks with artificial colors.
Transitioning from Clear Liquids: The Low-Fiber (Low-Residue) Diet
As your symptoms begin to improve, you’ll gradually transition to a low-fiber diet. This phase is crucial for allowing your colon to heal while still providing some nutrition. This part of the diverticulitis diet handout for patients focuses on easily digestible foods.
Foods to Include (Low-Fiber Phase):
- Refined Grains: White bread, white rice, white pasta, crackers made from refined flour.
- Cooked Vegetables (Peeled and Seedless): Well-cooked carrots, potatoes (without skin), zucchini (without seeds), asparagus tips.
- Fruits (Cooked and Seedless): Applesauce, canned peaches or pears (without skin), ripe bananas.
- Lean Proteins: Well-cooked chicken, turkey, fish, and eggs.
- Dairy (if tolerated): Yogurt (plain), milk (if tolerated).
Foods to Limit or Avoid (Low-Fiber Phase):
- Whole grains (whole wheat bread, brown rice, oats).
- Raw vegetables and fruits with skins and seeds.
- Legumes (beans, lentils, peas).
- Nuts and seeds.
- Popcorn.
- Spicy foods.
- Fried and greasy foods.
Reintroducing Fiber: The High-Fiber Diet for Prevention
Once you are symptom-free, the most important dietary strategy for preventing future diverticulitis flare-ups is to gradually increase your fiber intake. This is where the true power of this diverticulitis diet handout for patients lies – in long-term management.
The Magic of Fiber: Why It’s Your Best Friend
Fiber is indigestible plant material that plays a vital role in digestive health. It adds bulk to your stool, making it softer and easier to pass, which reduces pressure in the colon and helps prevent the formation of diverticula.
Gradual Fiber Increase: A Step-by-Step Approach
- Start Slowly: Don’t go from zero to sixty overnight! Suddenly increasing fiber can lead to gas, bloating, and discomfort. Add one high-fiber food at a time, every few days.
- Hydrate, Hydrate, Hydrate: Fiber absorbs water. Drinking plenty of fluids (at least 8 glasses of water a day) is essential for fiber to work effectively and prevent constipation.
- Listen to Your Body: Pay attention to how your body reacts to different foods. If a particular high-fiber food causes discomfort, reduce your intake or try a different source.
High-Fiber Foods to Embrace (Long-Term Management):
- Whole Grains: Whole wheat bread, whole grain pasta, brown rice, quinoa, oats, barley.
- Fruits: Berries (raspberries, blueberries, strawberries), apples (with skin), pears (with skin), oranges, prunes.
- Vegetables: Broccoli, Brussels sprouts, spinach, kale, sweet potatoes, corn, peas.
- Legumes: Lentils, black beans, kidney beans, chickpeas (start with small portions and ensure they are well-cooked).
- Nuts and Seeds: Almonds, walnuts, chia seeds, flaxseeds (in moderation and ensure adequate hydration).
Foods to Continue Limiting or Avoiding (Even in Remission):
While the focus shifts to fiber, it’s still wise to be mindful of certain foods that can be problematic for some individuals with diverticulitis.
- Red Meat: Some studies suggest a link between high red meat consumption and increased risk of diverticulitis.
- Processed Foods: Often low in fiber and high in unhealthy fats and sugar.
- High-Fat Foods: Can slow digestion and potentially contribute to discomfort.
- Spicy Foods: Can irritate the digestive tract for some.
- Alcohol: Can dehydrate and irritate the gut.
Beyond the Basics: Important Considerations for Your Diverticulitis Diet Handout for Patients
This diverticulitis diet handout for patients goes beyond just listing foods. Here are some additional tips to optimize your digestive health.
The Power of Probiotics
Probiotics are beneficial bacteria that can help maintain a healthy balance in your gut microbiome. Incorporating probiotic-rich foods can be particularly helpful after a course of antibiotics, which can sometimes disrupt gut flora.
Probiotic-Rich Foods:
- Yogurt: Look for yogurts with "live and active cultures."
- Kefir: A fermented milk drink.
- Sauerkraut and Kimchi: Fermented cabbage dishes.
- Kombucha: A fermented tea drink.
Hydration: Your Unsung Hero
Adequate fluid intake is absolutely critical for managing diverticulitis and ensuring your high-fiber diet works effectively. Dehydration can lead to harder stools, increasing the risk of constipation and potential pressure on the colon.
Tips for Staying Hydrated:
- Carry a water bottle with you throughout the day.
- Set reminders to drink water.
- Flavor your water with natural additions like cucumber, mint, or berries.
- Include water-rich foods like watermelon and cucumber in your diet.
Mindful Eating and Lifestyle Habits
Your diet is a significant piece of the puzzle, but it’s not the only one. Adopting healthy lifestyle habits can further support your digestive well-being.
Key Lifestyle Factors:
- Regular Exercise: Physical activity stimulates bowel function and can help prevent constipation.
- Stress Management: Stress can significantly impact digestive health. Explore techniques like meditation, yoga, or deep breathing exercises.
- Adequate Sleep: Aim for 7-9 hours of quality sleep per night.
- Chew Your Food Thoroughly: Proper chewing aids digestion and reduces the workload on your digestive system.
- Don’t Ignore the Urge: When you feel the need to have a bowel movement, don’t delay.
Sample Meal Plan: Putting Your Diverticulitis Diet Handout for Patients into Practice
To make this diverticulitis diet handout for patients even more practical, here’s a sample meal plan for the high-fiber phase. Remember to adjust portion sizes and specific foods based on your individual tolerance and preferences.
Day 1: A Fiber-Rich Celebration!
- Breakfast: Oatmeal made with rolled oats, topped with berries and a sprinkle of chia seeds. A glass of water.
- Lunch: Whole wheat turkey sandwich on whole grain bread with lettuce and tomato. A side of carrot sticks. Water.
- Snack: A pear with the skin on.
- Dinner: Baked salmon with roasted broccoli and quinoa. Water.
Day 2: Embracing Variety
- Breakfast: Scrambled eggs with spinach and a slice of whole wheat toast. Water.
- Lunch: Lentil soup (ensure well-cooked lentils) with a side salad of mixed greens and cucumber. Water.
- Snack: A small handful of almonds.
- Dinner: Chicken stir-fry with brown rice and a variety of colorful vegetables like bell peppers and snap peas. Water.
Day 3: Simple and Satisfying
- Breakfast: Greek yogurt with a sprinkle of granola and sliced peaches. Water.
- Lunch: Leftover chicken stir-fry. Water.
- Snack: An apple with the skin.
- Dinner: Whole wheat pasta with marinara sauce and lean ground turkey. A side of steamed green beans. Water.
When to Seek Professional Guidance
While this diverticulitis diet handout for patients provides valuable information, it’s crucial to remember that individual needs can vary. Always consult with your doctor or a registered dietitian for personalized advice, especially if you have underlying health conditions or are experiencing persistent symptoms. They can Eating well day heart healthy meal plan your ultimate guide to a vibrant heart help you create a tailored dietary plan that meets your specific needs and ensures you are getting adequate nutrition.
Frequently Asked Questions About Diverticulitis Diet
Q1: Are nuts and seeds really safe to eat with diverticulitis?
A: For most people in remission, nuts and seeds are safe and beneficial due to their fiber content. Historically, there was a concern they could get stuck in diverticula, but current research doesn’t support this. Start with small portions and ensure you’re well-hydrated. If you experience discomfort, discuss it with your doctor.
Q2: Can I drink alcohol with diverticulitis?
A: It’s generally recommended to limit or avoid alcohol, especially during a flare-up. Alcohol can dehydrate you and irritate your digestive system. In remission, moderate consumption might be acceptable for some, but it’s best to discuss this with your healthcare provider.
Q3: How quickly can I transition back to a normal diet after a flare-up?
A: The transition is gradual and depends on your individual recovery. You’ll typically start with clear liquids, then move to a low-fiber diet, and finally, slowly reintroduce fiber. Your doctor will guide you through this process.
Q4: What are the signs that my diverticulitis is flaring up again?
A: Common symptoms include abdominal pain (often in the lower left side), fever, nausea, vomiting, chills, and changes in bowel habits (constipation or diarrhea). If you experience these, contact your doctor immediately.
Q5: Is a diverticulitis diet handout for patients the same as a colonoscopy prep diet?
A: No, they are very different. A colonoscopy prep diet is a short-term, extremely restrictive diet designed to clear the colon for a medical procedure. A diverticulitis diet is a long-term management strategy focused on fiber intake and avoiding triggers.
Conclusion: Embrace Your Digestive Journey!
Managing diverticulitis is a journey, and this diverticulitis diet handout for patients is designed to empower you with the knowledge to make informed dietary choices. By embracing a fiber-rich diet, staying hydrated, and listening to your body, you can significantly improve your digestive health and enjoy a more comfortable, vibrant life. Celebrate the small victories, be patient with yourself, and remember that a well-nourished body is a happy body! Share this valuable information with others who might benefit from it, and let’s embark on a path to feeling fantastic together!